صياغة التميز في البرمجيات
دعنا نبني شيئاً استثنائياً معاً.
اعتمد على شركة Lasting Dynamics للحصول على جودة برمجيات لا مثيل لها.
ميشيل سيمينو
أبريل 03, 2026 • 9 min read

Pediatric oncology faces unique challenges that demand urgent innovation. Generative AI is now transforming how childhood cancers are diagnosed and treated, offering hope for better outcomes. With AI healthcare solutions advancing rapidly, personalized medicine and AI cancer treatment are becoming realities for young patients.
This shift matters now more than ever, as early detection and tailored therapies can save lives. Today we explore how generative AI is revolutionizing pediatric oncology from diagnosis to treatment plans.
Childhood cancer affects not only patients, but entire families who must navigate long periods of uncertainty, emotional stress, and complex medical decisions. Lasting Dynamics understands the seriousness of these situations and the responsibility that comes with working in the healthcare sector. For this reason, the company is committed to applying its experience in artificial intelligence in ways that are practical, responsible, and genuinely helpful for medical teams and caregivers.
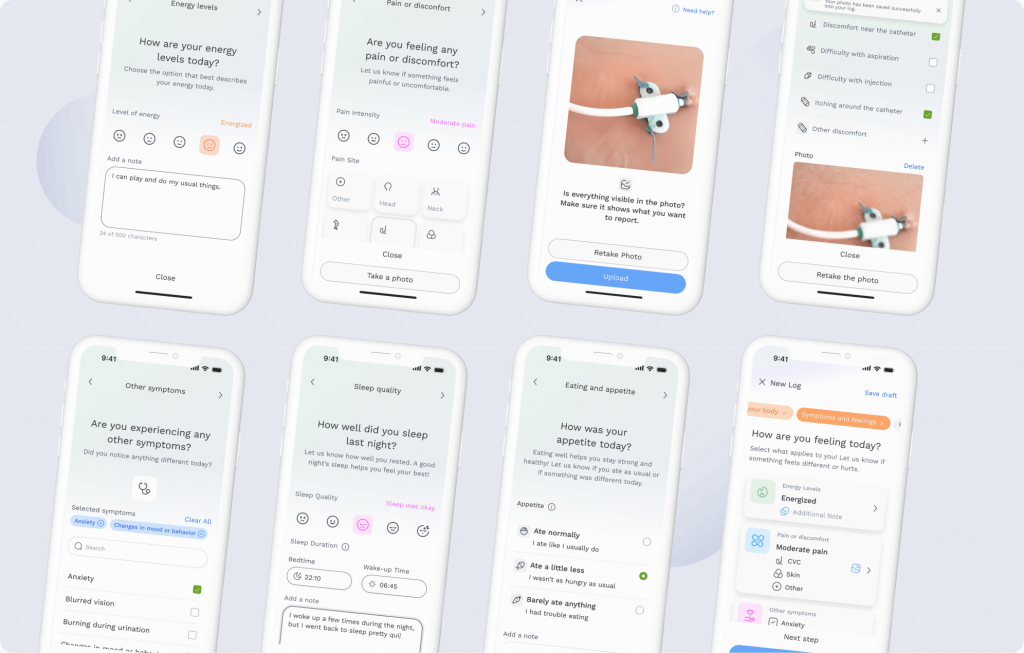
One of the projects that reflects this approach is الرضيع, a multidisciplinary platform designed to support clinical coordination in pediatric oncology as part of the MUSA initiative in Italy. INFANT enables collaboration between healthcare professionals through shared clinical spaces, multidisciplinary boards, and structured patient information, while also offering caregivers a mobile application to log daily symptoms and biometric data. AI components within the platform support clinical decision-making and information processing, helping teams work with complex data more effectively without adding unnecessary technical complexity.
In addition to الرعاية الصحية, Lasting Dynamics works across other sectors such as التمويل و sustainability. However, healthcare remains a key focus area due to its direct impact on people’s lives. Projects like INFANT are approached not simply as technical deliveries, but as long-term efforts to improve coordination, reduce friction in care processes, and support families and clinicians facing difficult circumstances. The goal is not innovation for its own sake, but meaningful technology that contributes to better outcomes and a better world.
"INFANT transformed how I coordinate with specialists and caregivers. It gave me one place to see the patient story unfold every log, every board, every update so I can focus more on care, less on chasing information."
د. لورينزو ف.، أخصائي أورام الأطفال
Let's start with some context. Pediatric oncology is a field marked by complexity and urgency. Childhood cancers often present differently than adult cancers, making early diagnosis difficult. Symptoms can be vague, and rare cancer types mean clinicians have limited data to draw from. This leads to delays in diagnosis, which can impact survival rates and long-term health outcomes.
Another major challenge is the variability in how children respond to treatments. Unlike adults, children’s bodies are still developing, so therapies must be carefully tailored to minimize side effects and long-term risks. The scarcity of large, high-quality datasets further complicates research and clinical decision-making, slowing progress in finding new cures and improving care.
And not only medical complexity, pediatric oncology also involves significant emotional and logistical challenges. Families often face long diagnostic journeys, uncertainty, and fragmented care across specialists and institutions. These factors place additional pressure on healthcare teams and highlight the need for more coordinated, data-driven approaches to diagnosis and treatment.
Generative AI is making significant strides in supporting early cancer detection in children. By analyzing vast amounts of medical data, including imaging, genetic profiles, and electronic health records, like AI systems can identify subtle patterns that may indicate cancer at its earliest stages. This enables clinicians to intervene sooner, improving the chances of successful treatment.
Clinical decision support systems powered by AI are also helping doctors make more accurate diagnoses. These tools can suggest possible conditions based on a child’s symptoms and test results, reducing diagnostic errors and ensuring that rare cancers are not overlooked. As a result, AI-powered pediatric cancer diagnosis is becoming a critical asset in modern healthcare.
دعنا نبني شيئاً استثنائياً معاً.
اعتمد على شركة Lasting Dynamics للحصول على جودة برمجيات لا مثيل لها.
Importantly, AI does not replace clinical judgment but boost it. By providing additional insights and risk indicators, AI supports clinicians in complex cases where experience alone may not be enough. This collaborative approach between technology and medical expertise helps build confidence in early diagnostic decisions.
One of the most promising applications of generative AI in pediatric oncology is treatment personalization. AI-driven models can analyze a child’s unique genetic makeup, tumor characteristics, and previous responses to therapy. This information allows oncologists to design personalized medicine strategies that maximize effectiveness while minimizing harmful side effects.
Personalized treatment plans are especially important for children, whose developing bodies are more sensitive to aggressive therapies. By leveraging AI, clinicians can select the most appropriate drugs, dosages, and treatment schedules, leading to better outcomes and improved quality of life for young patients.
Over time, these AI-informed treatment strategies also generate valuable feedback loops. As outcomes are monitored and fed back into the models, AI systems continuously improve, helping refine future treatment decisions and advancing precision medicine in pediatric cancer care.
Generative AI is already demonstrating its value in real-world pediatric oncology settings. For example, AI algorithms are being used to generate synthetic medical images for rare cancer types, helping to train diagnostic models even when real-world data is scarce. AI-powered tools are also assisting in the design of new clinical trials, identifying patient cohorts that are most likely to benefit from experimental therapies.
In addition, generative AI is enabling predictive modeling for treatment outcomes, allowing doctors and families to make more informed decisions about care. These use cases highlight the transformative potential of AI healthcare solutions in pediatric cancer treatment.
As these applications mature, generative AI is expected to play a broader role across the entire care continuum, from diagnosis and treatment planning to follow-up and survivorship monitoring, creating more consistent and proactive pediatric oncology workflows.
Despite its promise, the adoption of generative AI in pediatric oncology is not without challenges. One major pain point is data access. Medical data is often siloed across different institutions, making it difficult to aggregate the large datasets needed to train effective AI models. Privacy concerns are heightened when dealing with children’s health information, requiring robust safeguards and compliance with regulations like GDPR and HIPAA.
Integration with existing healthcare systems is another hurdle. Many hospitals and clinics use legacy software that is not compatible with modern AI tools, leading to workflow disruptions and resistance from staff. Overcoming these challenges is essential to unlocking the full potential of AI in pediatric oncology.
بدءاً من الفكرة إلى الإطلاق، نقوم بتصميم برامج قابلة للتطوير مصممة خصيصاً لتلبية احتياجات عملك.
شارك معنا لتسريع نموك.
Addressing these pain points requires not only technical solutions, but also organizational alignment. Clear governance, interoperability standards, and trust between institutions are critical to enabling secure data sharing and sustainable AI adoption.
Generative AI delivers substantial business value for healthcare providers, patients, and organizations. By automating routine tasks and supporting clinical decision-making, AI increases efficiency and allows medical staff to focus on complex cases. Improved diagnostic accuracy reduces the risk of costly errors and unnecessary treatments, while personalized medicine strategies can lower the overall cost of care by targeting therapies more effectively.
For healthcare organizations, investing in AI healthcare solutions can lead to better patient outcomes, higher satisfaction rates, and a stronger reputation in the market. These benefits make a compelling case for adopting generative AI in pediatric oncology.
In the long term, AI-driven efficiencies can also support more sustainable healthcare systems. Optimized resource allocation, reduced hospital stays, and better treatment planning contribute to both economic and operational resilience.
The use of AI in pediatric oncology raises important ethical questions. Ensuring that AI models are transparent, explainable, and free from bias is critical, especially when making life-altering decisions for children. Informed consent and data privacy must be rigorously maintained, with clear communication to families about how AI is being used in their child’s care.
There is also a responsibility to ensure equitable access to AI-powered treatments, so that all children, regardless of background or location, can benefit from the latest advances in cancer care. Addressing these ethical considerations is essential for building trust and ensuring the responsible use of AI in healthcare.
Ethical AI governance should be embedded from the start, combining clinical oversight, technical validation, and patient-centered values. This approach helps ensure that innovation progresses without compromising safety or fairness.
Successful implementation of generative AI in pediatric oncology requires close collaboration between clinicians, data scientists, and technology experts. Multidisciplinary teams are essential for developing, validating, and deploying AI tools that meet the unique needs of pediatric patients. This collaborative approach ensures that AI solutions are clinically relevant, user-friendly, and seamlessly integrated into existing workflows.
Ongoing training and support for healthcare staff are also crucial. By fostering a culture of innovation and continuous learning, organizations can maximize the impact of AI in pediatric cancer care.
نحن نصمم ونبني منتجات رقمية عالية الجودة ومميزة.
الموثوقية والأداء والابتكار في كل خطوة.
When collaboration is done well, AI becomes a natural extension of the care team rather than an external tool. This alignment between people, processes, and technology is key to achieving meaningful and lasting improvements in pediatric oncology outcomes.

Generative AI is delivering clear and measurable benefits in pediatric oncology. Earlier and more accurate cancer detection enables faster intervention, while personalized treatment plans allow therapies to be tailored to each child’s unique biological profile. AI-driven efficiency also reduces administrative burdens on clinicians, freeing up time for patient care, and improves predictive modeling for treatment outcomes. At the same time, AI expands access to advanced therapies and clinical trials, helping connect patients with cutting-edge treatment options that were previously difficult to reach.
However, these benefits come with significant challenges. Limited access to high-quality, diverse pediatric data restricts the training of reliable AI models, while strict privacy and regulatory requirements demand strong governance frameworks. Integration with legacy healthcare IT systems remains complex, and many institutions struggle to adopt modern AI tools without disrupting existing workflows. Ensuring transparency and explainability of AI models is also critical to maintaining clinical trust and accountability.
Now, this is important to remember, these benefits coexist with notable challenges. Limited access to high-quality, diverse pediatric datasets restricts model accuracy and generalizability. Strict privacy regulations and ethical obligations demand robust safeguards, particularly when handling children’s health data. Integration with legacy healthcare IT systems often creates technical and workflow barriers, while ensuring transparency and explainability remains essential for clinical trust.
The future of generative AI in pediatric oncology is bright. Advances in machine learning, natural language processing, and data integration are paving the way for even more powerful diagnostic and treatment tools. In the next 5–10 years, we can expect to see AI playing a central role in early cancer detection, real-time monitoring of treatment responses, and the development of novel therapies.
Ongoing research and collaboration between healthcare providers, technology companies, and regulatory bodies will be key to realizing this vision. As AI continues to evolve, its impact on pediatric oncology will only grow, offering new hope to children and families affected by cancer.
In the long term, AI is likely to become a foundational layer of pediatric healthcare infrastructure. Rather than being a standalone innovation, it will operate as an integrated intelligence system across hospitals, research centers, and care networks, supporting prevention, diagnosis, treatment, and long-term survivorship in a more connected and proactive model of care.
Generative AI is redefining how pediatric oncology is understood and practiced. From early diagnosis and personalized treatment to predictive modeling and clinical decision support, AI is transforming complex, fragmented processes into more connected and data-driven care pathways. Its value lies not only in technological advancement, but in its ability to support clinicians, empower families, and improve outcomes for children facing cancer.
At the same time, the responsible adoption of AI requires careful attention to ethics, data governance, system integration, and human collaboration. Trust, transparency, and explainability are as important as accuracy and performance. Without strong foundations in privacy, interoperability, and multidisciplinary cooperation, even the most advanced AI systems risk failing to deliver real-world impact.
To conclude, the future of pediatric oncology will not be defined by AI alone, but by how well it is integrated into human-centered care models. When technology, clinical expertise, and ethical responsibility align, generative AI becomes more than an innovation, it becomes a catalyst for safer, more equitable, and more effective cancer care for children worldwide.
Ready to transform pediatric oncology with generative AI? 👉 للتواصل مع Lasting Dynamics for a consultation and discover how our AI healthcare solutions can help you deliver better outcomes for children and families.
Generative AI is used to analyze complex medical data such as imaging, genomic information, and electronic health records. It supports earlier and more accurate diagnosis, helps personalize treatment plans, and enables predictive modeling to assess treatment responses, supporting clinicians in making more informed decisions.
AI improves pediatric cancer care by enabling earlier detection, increasing diagnostic accuracy, and supporting personalized treatment strategies. It also increase clinical efficiency by reducing administrative workload, improving decision-making processes, and allowing healthcare professionals to focus more on patient-centered care.
Yes, privacy is a critical concern in pediatric healthcare. AI solutions must comply with strict data protection regulations such as GDPR and HIPAA, ensuring secure data handling, transparency, and ethical use. Strong governance frameworks are essential to protect sensitive children’s health information.
Hospitals should begin by assessing their existing data infrastructure and identifying clinical areas where AI can add value. Partnering with experienced AI solution providers like Lasting Dynamics helps ensure proper integration, regulatory compliance, and the development of AI tools aligned with real clinical workflows.
Organizations often face challenges related to limited access to high-quality data, regulatory compliance, and integration with legacy systems. Additional barriers include ensuring model transparency, managing change within clinical teams, and providing adequate training to support effective and sustainable AI adoption.
حوّل الأفكار الجريئة إلى تطبيقات قوية.
Let’s create software that makes an impact together.
ميشيل سيمينو
أؤمن بالعمل الجاد والالتزام اليومي كوسيلة وحيدة للحصول على النتائج. أشعر بجاذبية لا يمكن تفسيرها للجودة وعندما يتعلق الأمر بالبرمجيات فهذا هو الدافع الذي يجعلني وفريقي نتمسك بشدة بممارسات أجايل والتقييمات المستمرة للعمليات. لديّ موقف تنافسي قوي تجاه كل ما أتناوله - بطريقة لا أتوقف فيها عن العمل، حتى أصل إلى القمة، وبمجرد أن أصل إلى القمة، أبدأ العمل للحفاظ على مكانتي.